The pulmonary form of anthrax, due to inhalation of spores, is the most dangerous manifestation of the disease. Pneumonia-like symptoms develop, and the organisms may invade the bloodstream and even the brain. The fatality rate is greater than 90%. Under usual circumstances, pulmonary anthrax is rare, found mainly among people who work with wool or fleeces. Viable, vegetative forms of Bacillus anthracis, although microscopic, are too large to readily enter the alveoli (air sacs) of the human lung. However, the spores are much smaller, and can gain entry to the alveoli, germinate, produce toxic substances, and cause disease.
This characteristic of Bacillus anthracis spores, plus the high resistance to environmental stress, makes these bacteria ideal agents for biological warfare. Large-scale production and dispersal of Bacillus anthracis spores has the potential for causing high mortality in a target population. On the positive side, however, is the fact that dispersal of spores can be difficult, and it takes about 10,000 spores to initiate an infection. This latter fact may contribute to the fact that anthrax is not considered to be communicable.
Inhalation form
3. GASTROINTESTINAL FORM
Ingestion of Bacillus anthracis, or its spores, can result in intestinal anthrax; the form most commonly seen in animals. The clinical signs are pain, vomiting, and bloody diarrhea. This form of the disease has a 25% to 50% fatality rate. Eating undercooked meat that is infected with the anthrax bacteria, or drinking unchlorinated water that harbors the spores, can introduce the bacteria into the gastrointestinal tract. Infection can occur in either the upper or lower GI tract. This form of anthrax is rare.
GI form
How anthrax attacks?
Taken from Yale University
The virulence of B. anthracis lies not in the bacterium itself but rather in the toxins it produces. The three major toxins released by B. anthracis are proteins known as Protective Antigen (PA), Edema Factor (EF), and Lethal Factor (LF), which work together to kill blood cells. As part of a normal immune response, a macrophage first engulfs a spore, which quickly germinates. As active bacteria burst out of the macrophage, they release PA. PA attaches to the surface of a T-cell, interacting with the cell membrane to form vesicles that can transport EF and LF into the cytoplasm. Once inside, the cyclase EF overwhelms the cell by producing massive amounts of signaling protein cAMP. The protease LF, on the other hand, destroys the MAP kinases’ signaling proteins, thereby disrupting cell cycle regulation and killing the cell. Without T-cells, the body cannot effectively combat the intruders and falls severely ill.
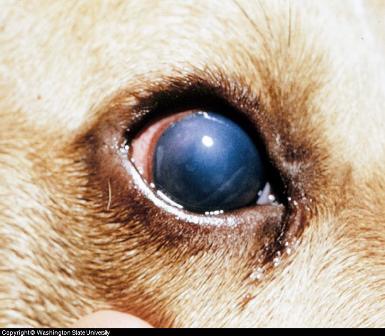
Clinical findings in animals
Typically, the incubation period is 3-7 days (range 1-14 days). The clinical course ranges from peracute to chronic. The peracute form (common in cattle and sheep) is characterized by sudden onset and a rapidly fatal course. Staggering, dyspnea, trembling, collapse, a few convulsive movements, and death may occur in cattle, sheep, or goats with only a brief evidence of illness.
In acute anthrax of cattle and sheep there is an abrupt fever and a period of excitement followed by depression, stupor, respiratory or cardiac distress, staggering, convulsions, and death. Often, the course of disease is so rapid that illness is not observed and animals are found dead. The body temperature may reach 107F (41.5C), rumination ceases, milk production is materially reduced, and pregnant animals may abort. There may be bloody discharges from the natural body openings. Some (chronic?) infections are characterized by localized, subcutaneous, edematous swelling that can be quite extensive. Areas most frequently involved are the ventral neck, thorax, and shoulders.
The disease in horses may be acute. Signs may include fever, chills, severe colic, anorexia, depression, weakness, bloody diarrhea, and swellings of the neck, sternum, lower abdomen, and external genitalia. Death usually occurs within 2-3 days of onset.
Although relatively resistant, pigs may develop an acute septicemia following ingestion of B anthracis , characterized by sudden death, oropharyngitis, or more usually a mild chronic form. Oropharyngeal anthrax is characterized by rapidly progressive swelling of the throat, which may cause death by suffocation. In the chronic form, pigs show systemic signs of illness and gradually recover with treatment. Some later show evidence of anthrax infection in the cervical lymph nodes and tonsils when slaughtered (as apparently healthy animals). Intestinal involvement is seldom recognized and has nonspecific clinical characteristics of anorexia, vomiting, diarrhea (sometimes bloody), or constipation.
Lesions
Rigor mortis is frequently absent or incomplete. Dark blood may ooze from the mouth, nostrils, and anus with marked bloating and rapid body decomposition. If the carcass is inadvertently opened, septicemic lesions are seen. The blood is dark and thickened and fails to clot readily. Hemorrhages of various sizes are common on the serosal surfaces of the abdomen and thorax as well as on the epicardium and endocardium. Edematous, red-tinged effusions commonly are present under the serosa of various organs, between skeletal muscle groups, and in the subcutis.
Hemorrhages frequently occur along the GI tract mucosa, and ulcers, particularly over Peyers patches, may be present. An enlarged, dark red or black, soft, semifluid spleen is common. The liver, kidneys, and lymph nodes usually are congested and enlarged. Meningitis may be found if the skull is opened.
In pigs with chronic anthrax, the lesions usually are restricted to the tonsils, cervical lymph nodes, and surrounding tissues. The lymphatic tissues of the area are enlarged and are a mottled salmon to brick-red color on cut surface. Diphtheritic membranes or ulcers may be present over the surface of the tonsils. The area around involved lymphatic tissues generally is gelatinous and edematous. A chronic intestinal form involving the mesenteric lymph nodes is also recognized.
Diagnosis
Specific diagnostic tests include bacterial culture, PCR tests, and fluorescent antibody stains to demonstrate the agent in blood films or tissues. Western blot and ELISA tests for antibody detection are available in some reference laboratories. Lacking other tests, fixed blood smears stained with Loefflers or MacFadean stains can be used and the capsule visualized; however, it can result in some 20% false positives.
Differential diagnosis
Peracute blackquarter (clostridium chauvoi) and septicaemic form of other diseases. In splenic enlargement as seen in babesiosis, anaplasmosis and leucosis, spleen consistency is firm. In anthrax, the spleen is soft and upon incision the pulp exudes like thick blackish-red blood.
Treatment in animal
Early treatment and vigorous implementation of a preventive program are essential to reducing losses among livestock. Livestock at risk should be immediately treated with a long-acting antibiotic to stop all potential incubating infections. Domestic livestock respond well to penicillin if treated in the early stages of the disease. Oxytetracycline given daily in divided doses also is effective. Other antibacterials, including amoxicillin, chloramphenicol, ciprofloxacin, doxycycline, erythromycin, gentamicin, streptomycin, and sulfonamides also can be used, but their effectiveness in comparison with penicillin and the tetracyclines has not been evaluated under field conditions.
Control in animal
Anthrax is controlled through vaccination programs, rapid detection and reporting, quarantine, treatment of asymptomatic animals (postexposure prophylaxis), and burning or burial of suspect and confirmed cases. In livestock, anthrax can be controlled largely by annual vaccination of all grazing animals in the endemic area and by implementation of control measures during epizootics. The nonencapsulated Sterne-strain vaccine is used almost universally for livestock immunization. Vaccination should be done 2-4 wk before the season when outbreaks may be expected. Because this is a live vaccine, antibiotics should not be administered within 1 wk of vaccination. Before vaccination of dairy cattle during an outbreak, all of the procedures required by local laws should be reviewed and followed.

In addition to therapy and immunization, specific control procedures are necessary to contain the disease and prevent its spread. These include the following:
1) notification of the appropriate regulatory officials
2) rigid enforcement of quarantine (after vaccination, 2 wk before movement off the farm, 6 wk if going to slaughter)
3) prompt disposal of dead animals, manure, bedding, or other contaminated material by cremation (preferable) or deep burial
4) isolation of sick animals and removal of well animals from the contaminated areas
5) cleaning and disinfection of stables, pens, milking barns, and equipment used on livestock
6) use of insect repellents
7) control of scavengers that feed on animals dead from the disease; and
8) observation of general sanitary procedures by people who handle diseased animals, both for their own safety and to prevent spread of the disease.
Contaminated soils are very difficult to completely decontaminate, but formaldehyde will be successful if the level is not excessive. The process generally requires removal of soil.
Sources: How Anthrax works; Lee Ann Obringer, Hijacking nature's agents; Andrew Chang Yale Scientific, Anthrax; VETNEXT, Anthrax in human; www.medicine.net.com. Anthrax in animals; ww.foa.org