Let refresh physiology! kudos to Prof Noordin!
***************************************************
Circulatory disturbances
Any interference with the blood flow to a portion of the body results in a circulatory disturbance. Homeostasis must be corrected in order to keep the body system well.
Homeostasis - Normal fluid homeostasis encompasses maintenance of vessel wall integrity as well as intravascular pressure and osmolarity within certainphysiologic ranges. It is also means maintaining blood as a liquid until injury causing clot formation. Clotting at the inappropriate site (thrombus), or migration of clot (embolism), obstruct blood flow to tissues and leads to cell death (infarction). Conversely inability to clot after injury results in haemorrhage. Extensive haemorrhage can cause shock.
There are 6 types of circulatory disturbances;
1. Hyperraemia
2. Congestion
3. Thrombus
4. Emboli
5. Haemorrhage
6. Infraction
Hyperaemia
Hyperaemia is the increase in blood flow in an organ or tissue due to dilatation of arteries or arteriole. Hyperaemia is an active process especially in inflammation where redness can be seen under the skin clearly.
Eg Physiology hyperraemia: In skeletal and cardiac muscle in muscular exercise in splanchnic area after eating.
Eg Pathological hyperraemia: In acute inflammation
Usually, hyperaemia results in erythema

Normal vs hyperaemia
The skin will appear red as the results of active blood flow
Congestion
Congestion is passive hyperaemia due to engorgement of veins and venules by blood. Usually there are 3 examples of congestion. Systemic venous congestion, Pulmonary congestion, and localized venous congestion.
Systemic venous congestion: Blood accumulates in pulmonary veins all over the body of congestive heart failure of sparing the lung in case of right side of heart failure.
Pulmonary congestion: Blood accumulates in pulmonary veins and their tributaries in the case of left side of heart failure or mitral stenosis
Localized VC: Due to obstruction to blood flow in a limited area or an organ

Normal vs congestion
Edema is an classic example of congestion. Edema is the accumulation of access fluid in the interstitial tissue spaces or body cavity. 5 pathophysilogic mechanism that underlie the development of edema are
1. Decrease oncotic pressure-liver cirrhosis, malnutrition, nephrotic syndrome
2. Increase hydrostatic pressure- congestive heart failure, constrictive pericarditis, venous obstruction
3. Lymphatic obstruction- inflammatory, neoplastic, post surgical
4. Increase vascular permeability (e.i inflammation)
5. Sodium retention-renal insufficiency, increase renin-angiotensin-aldesterone secretion
Edema can occur in various organs such as lungs, skin, liver, brain, spleen and kidney

How edema occurs



Edema in lung. Note that the left picture showing the alveolar spaces is filled with red blood cell
Thrombus
Formation of blood clot (thrombus) in uninjured vessels or thrombic occlusion of a vessel after minor injury. The thrombus if formed of blood elements essentially platelets that develop inside the CVS during LIFE!!
how thrombus occur?

1. Endothelial injury

2.Hypercoaglability
Any alteration of the coagulation pathways that predispose to thrombosis. Eg genetics and sickle cell anemia
3. Abnormal blood flow
Can cause disrupt the laminar flow bringing platelets into contact with endothelium, promote endothelial cell activation, prevent dilution of the activated clotting factors by fresh flowing blood, retard the inflow clotting factors inhibitors--->thrombus formation

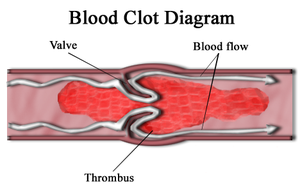
Venous thrombus
eg: Deep vein thrombosis (DVT)
Fate of a thrombus
Propagation- Thrombi may accumulate more platelets and fibrin eventually obstructing other critical vessel
Dissolution- Thrombi may be removef by fibriolytic activity
Embolisation-Detach thrombi from vessels may migrate and block small capillaries (emboli)
Organisation and Recanalisation- Thrombi may induce inflammation and fibrosis (organization) and may eventually recanalize
Infection forming mycotic aneurysm and septic embolisation
Embolism
A detached intravascular solid, liquid or gaseous mass that is carried by the blood to a site distant from its point of origin99% of the emboli are dislodged thrombi, hence, the term THROMBOEMBOLISM. Potential consequence of embolism is INFARCTION of the tissue distal to it.

Process of embolism
TypesThromboembolism
Fat embolism eg after fractures
Air embolism, eg in open carotid injury, angiographic procedures, Caisson’s disease in deep sea divers
Amniotic fluid embolism in abruption placenta of pregnancy
Emboli in brain
Infraction
Area of ischemic necrosis caused by occlusion of either the arterial supply or the venous drainage in a particular tissue.
Example
- Myocardial Infraction
- stroke
- pulmonary infarct following PTE
- gangrene of limbs due to PVD
- tortion of testes causing testicular infarction
- volvulus intussusception causing bowel gangrene
- Nature of blood supply
- Lungs have dual supply from pulmonary and bronchial arteries
- Liver has dual supply from hepatic artery and portal vein
- Kidney, spleen and brain have end arteries with no anastomosis
Rate of occlusion: if slow, can allow for collateral formation, eg in coarctation of aorta
Tissue vulnerability to hypoxia: neural tissue is the most susceptible, dying within 3 to 4 minutes, and myocardium within 30 to 40 min
Gross Morphology:
Infarction starts as a poorly defined wedge shaped area, with exudates and hemorrhagic area, which gets more defined by a rim of inflammation after some days.
2 types of infraction (based on their appearance)
Red infarct
Filled with blood. Characterized by coagulation necrosis and erythrocytes from adjacent arteries and veins. Seen with venous occlusions or within loose tissue that allow blood to collect in the infarcted zone of in organs with dual blood supply (lung, liver) or extensive collateral circulation (brain, smallintestine). The latter results because blood flows from the unobstructed vascular
channels into the necrotic area.
Red infact
White infarct
Lacks blood, also called anemic infarct. (Usually has a red zone at periphery because of capillaries at the border of infarct undergo dissolution and blood seeps into the area of necrosis). Occurs with arterial occlusions in solid organs (heart, kidney).
Area of infarct in spleen
Haemorrhage
Escape of blood from the cardiovascular system (extravasation).Discharge of blood from the vascular compartment to the exterior of the body orenclosed within a tissue. Capillary bleeding can occur under conditions of chroniccongestion.
Causes
- Trauma
- subcutaneous or intramuscular hemorrhage
- Septicemia, viremia or toxic conditions
- widespread petechiae and ecchymoses
- Coagulation Disorders
- hemorrhage thrombocytopenia (decreased numbers of platelets)
Origin of hemorrhage
Hemorrhage by rhexis: due to substantial rant or tear present in the blood vessel or heart. Moderate flow of blood out from vascular system
Hemorrhage by diapedisis: due to small defect or rbc passing through the wall in hyperaemia of inflammation
Types of hemorrhage (according to sizes)
1.Petechiae- pin-point foci of haemorrhage up to 1-2 mm in size
2.Purpura- Hemorrhages 3mm. May be associated with diseases which cause petechiae, vascular inflammation or vascular damage. Often scattered on many body surfaces.
Purpura
3. Echymoses- Larger than petechiae and usually blotchy or irregular areas up to >1-2 cm in size often seen with trauma and other problems. (eg: subcutaneous hematomas / bruises)
Echymoses
4. Hematoma- Mass of fibrin and red cells surrounded by vascular connective tissue (supplies nutrients and support for phagocytes (macrophages)
Hematoma
Sources: MBBS Medicine.blogspot.com, circulatory disturbance; docslide.com, circulatory of disturbance; Lisa Miller, General Pathology VPM 152
Ps: This is incomplete article. More references needed




















1 comments:
Great information. Thank you for sharing
Download Indian Doctors Networkwhere you can network and communicate with executive committee members, senior doctors and mentors.
Post a Comment